Is Mohs Surgery or Radiation Therapy the Best Treatment for Skin Cancer?


Mohs surgery and radiation therapy are both effective for treating skin cancer, but they work very differently. Mohs surgery removes cancer layer by layer with real-time microscopic examination, offering up to 99% cure rates and maximum tissue preservation, while radiation therapy damages cancer cells over multiple sessions but affects surrounding healthy tissue and can cause long-term skin changes. For most basal cell and squamous cell carcinomas, especially on the face, Mohs surgery remains the more precise and preferred option.
Understanding the Differences Between Mohs Surgery and Radiation Therapy
Skin cancer is the most common cancer in the United States, and when detected early, it’s highly treatable. Two common treatment options, Mohs micrographic surgery and radiation therapy, offer effective outcomes, but in very different ways. While both can remove or control skin cancer, Mohs surgery remains the gold standard for many cases because of its exceptional precision, cure rate, and tissue preservation. Understanding how these treatments differ helps patients make informed, confident decisions about their care.
Introduction to Skin Cancer
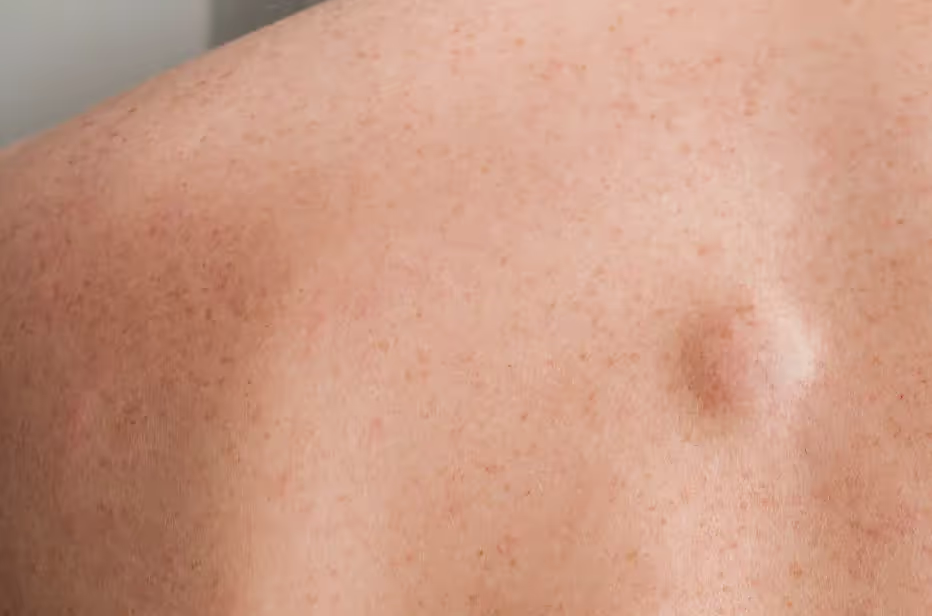
Skin cancer is the most common form of cancer, affecting millions of people each year. It develops when abnormal cells in the skin grow uncontrollably, often as a result of cumulative sun exposure. The two most common types of skin cancer are basal cell carcinoma and squamous cell carcinoma, both classified as nonmelanoma skin cancers. Actinic keratosis is a common, sun-induced, pre-cancerous skin lesion that appears as rough, scaly patches, mainly on sun-exposed skin such as the face and hands, and can develop into skin cancer if left untreated.
Basal cell carcinomas account for the majority of cases, while squamous cell carcinomas are the second most frequent. These cancers typically arise on sun-exposed areas of the skin, such as the face, ears, neck, and hands—areas of sun-exposed skin. Early detection is key, as most skin cancers, including squamous cell skin cancer that can invade deeper skin layers if not caught early, can be effectively treated when caught in their initial stages.
One of the most advanced and effective treatments for these cancers is Mohs micrographic surgery, which is designed to remove all cancerous cells while preserving as much healthy tissue as possible. This tissue-sparing approach is especially important for maintaining both the function and appearance of the skin, and is particularly used for cutaneous squamous cell carcinoma.
Understanding Basal Cell Carcinoma
Basal cell carcinoma, the most common form of skin cancer, begins in the basal cell layer, which is the deepest part of the epidermis—the outermost layer of the skin. Basal cell carcinomas most often appear on areas of the skin that receive the most sun exposure, such as the face, ears, neck, and hands. While basal cell carcinoma typically grows slowly and rarely spreads to other parts of the body, it can cause significant local damage if left untreated, sometimes invading nearby tissues and structures.
Because of its potential to cause disfigurement, especially on visible or delicate areas, early detection and prompt treatment are essential. Mohs surgery is considered one of the most effective treatments for basal cell carcinoma, particularly for high risk or complex cases where preserving healthy tissue is crucial. By removing the cancer layer by layer and examining each under a microscope, Mohs surgery ensures that all cancerous cells are eliminated while sparing as much healthy skin as possible. This approach not only maximizes the chances of a cure but also helps maintain the appearance and function of the affected area. If you notice a new or changing spot on your skin, especially in sun-exposed areas, it’s important to have it evaluated by a dermatologist to rule out basal cell carcinoma or other types of skin cancer.
Risk Factors for Skin Cancer
Understanding your risk factors for skin cancer can help you take proactive steps to protect your health. Both basal cell carcinoma and squamous cell carcinoma share several common risk factors. Prolonged exposure to ultraviolet (UV) radiation from the sun or tanning beds is the leading cause of most skin cancers. People with fair skin, blond or red hair, and light-colored eyes are at higher risk because they have less natural protection against UV rays. A personal or family history of skin cancer also increases your risk, as does having a large number of moles or atypical moles.
Certain medical conditions and treatments can further elevate your risk. Individuals who have undergone an organ transplant and are taking immunosuppressive medications are more likely to develop skin cancer, including both basal cell carcinoma and squamous cell carcinoma. Genetic conditions, such as basal cell nevus syndrome, can also predispose individuals to developing multiple basal cell cancers. Additionally, exposure to specific chemicals like arsenic has been linked to a higher risk of skin cancer. By being aware of these risk factors, you can take steps to reduce your chances of developing skin cancer and seek early evaluation for any suspicious changes in your skin.
What Is Mohs Micrographic Surgery?
Mohs surgery, also called Mohs micrographic surgery, is a specialized technique that removes skin cancer layer by layer while preserving as much healthy tissue as possible. The area is numbed with a local anesthetic, and local anesthesia is used so the patient remains comfortable and awake throughout the Mohs procedure. It’s performed by specially trained Mohs surgeons, who act as both the surgeon and the pathologist during the procedure. In each stage, the surgeon removes a thin layer of fresh tissue from the affected skin, which is then immediately examined under a microscope to check for any remaining cancer cells.
During the procedure, the patient waits between stages while the tissue is examined. If cancer is still present, only the specific area where it remains is removed. This process continues until all margins are clear, ensuring complete removal while sparing healthy tissue, including important structures like hair follicles.
Because the Mohs surgeon checks every layer in real time, Mohs surgery offers the highest level of precision available in skin cancer treatment. It’s particularly valuable for common skin cancers such as basal cell skin cancer and squamous cell skin cancers, which originate in squamous cell skin and squamous cells, as well as for tumors that may arise from hair follicles. Mohs surgery is especially important for treating cancers on the face, scalp, neck, or hands—areas where preserving normal skin is crucial for both function and appearance.
Risks and Complications of Mohs Surgery
While Mohs micrographic surgery is widely recognized for its safety and effectiveness in treating skin cancer, it is important to be aware of potential risks and complications. The overall complication rate for Mohs surgery is extremely low. The most common issues include minor infections at the surgical site, bleeding, hematoma (a collection of blood under the skin), and problems with wound healing such as dehiscence (wound reopening) or ischemic necrosis (tissue not getting enough blood supply).
It is also important to note that there are absolute contraindications to Mohs surgery. Specific health conditions or tumor features may make the procedure inadvisable or unsafe, and your surgeon will evaluate for these absolute contraindications to ensure patient safety and optimal outcomes. By discussing your medical history and medications with your Mohs surgeon, you can help ensure the safest possible outcome.
How Radiation Therapy Works for Skin Cancer
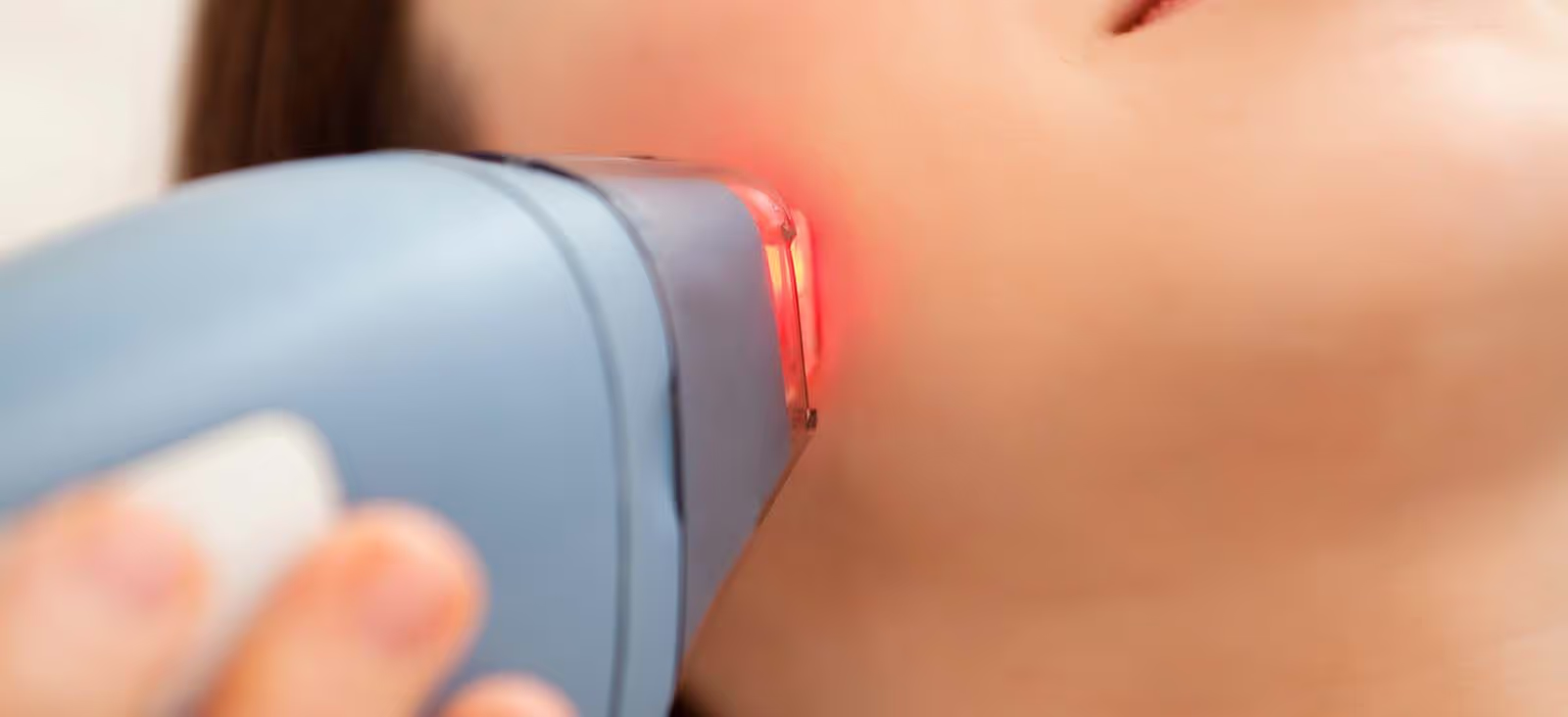
Radiation therapy treats skin cancer by using controlled beams of energy to destroy cancer cells. It can be effective for patients who cannot undergo surgery due to medical reasons, or for tumors in locations where surgery might be complex. Radiation therapy is commonly used to treat various types of cell skin cancer, including those originating in specific skin cell layers. The treatment is delivered over a series of sessions, typically spread across several weeks.
Unlike Mohs surgery, radiation does not remove the cancerous tissue; instead, it damages the DNA inside the cancer cells, preventing them from growing or dividing. Over time, the treated area heals as the body clears the damaged cells. However, because radiation affects not only the cancer cells but also the surrounding healthy tissue, it is less site-specific. The energy field must include a safety margin around the visible tumor, which means that more skin is treated than may be necessary.
This lack of precision can lead to several long-term skin changes. Radiation can thin the skin, weaken its structure, and cause scarring or pigment alterations that become more noticeable months or years later. The skin may also lose elasticity, develop chronic redness, or heal more slowly after future injuries or procedures in that area.
Why Mohs Surgery Is Often the Preferred Option
Mohs surgery remains the most precise and effective treatment for many non-melanoma skin cancers. Because it combines surgical removal with immediate microscopic analysis, it ensures that all cancer cells are completely removed, leaving the patient cancer free at the end of the procedure while sparing healthy tissue. This leads to a cure rate of up to 99% for primary basal and squamous cell carcinomas, which is higher than any other treatment method.
Another major advantage of Mohs surgery is tissue preservation. By removing only the skin that contains cancer, it leaves behind as much normal tissue as possible. This focus on tissue conservation is a key benefit of Mohs surgery, especially for visible or functionally sensitive areas—such as the nose, eyelids, lips, and ears—where even a small difference in tissue loss can significantly impact both appearance and healing. The result is typically smaller scars and a more natural cosmetic outcome.
Mohs surgery also offers immediate confirmation that the cancer has been fully removed. Patients receive their results as the surgery progresses, rather than waiting weeks to see if radiation has been effective. This step-by-step approach minimizes uncertainty and reduces the likelihood of recurrence.
Limitations of Radiation Therapy
While radiation therapy is valuable in specific cases, such as for patients who cannot tolerate surgery or for tumors in difficult locations, it has several limitations compared to Mohs surgery.
Radiation requires multiple treatments over an extended period, and its results are not immediate. Because it treats both the cancer and a margin of healthy skin, the procedure is not as precisely targeted as Mohs surgery. The surrounding tissue can sustain collateral damage, leading to skin thinning, discoloration, scarring, and long-term fragility. These changes may not appear right away but can develop gradually, sometimes years after treatment.
Additionally, cancers that recur in areas previously treated with radiation can be more challenging to manage surgically due to scarring and tissue changes. Mohs surgery is often recommended for lesions that have recurred after previous treatment, as its precision allows for effective removal of cancer in scarred or altered tissue. For this reason, Mohs surgery is generally recommended for primary tumors and recurrent lesions whenever possible.
Preventing Skin Cancer
Skin cancer prevention is a lifelong commitment that can significantly reduce your risk of developing basal cell carcinoma, squamous cell carcinoma, and other types of skin cancer. The American Academy of Dermatology recommends several key strategies for protecting your skin. Always use a broad-spectrum sunscreen with an SPF of 30 or higher, even on cloudy days, and reapply it every two hours when outdoors. Wearing protective clothing, such as wide-brimmed hats, long sleeves, and sunglasses, adds an extra layer of defense against harmful UV rays. Seek shade during peak sun hours, typically between 10 a.m. and 4 p.m., and avoid the use of tanning beds, which can dramatically increase your risk of skin cancer.
Regular self-examinations are also vital for early detection. Check your skin monthly for any new growths, changes in existing moles, or spots that look different from the rest. If you notice anything unusual, schedule an appointment with a dermatologist promptly. Individuals at high risk—such as those with a history of skin cancer, fair skin, or a weakened immune system—should see a dermatologist regularly for professional skin checks. By following these skin cancer prevention tips and staying vigilant, you can help protect your skin and catch any potential problems early, when they are most treatable.
Care After Skin Cancer Treatment
Proper care after skin cancer treatment, including Mohs surgery, is essential for optimal healing and long-term skin health. After the procedure, your surgeon will cover the surgical site and provide detailed instructions on wound care, which may include applying topical ointments or prescription medicines to promote healing and prevent infection. It’s important to follow these instructions closely and attend all scheduled follow-up appointments so your healthcare team can monitor your recovery.
For larger or more complex wounds, reconstructive surgery may be required immediately after Mohs surgery. Depending on the size and location of the defect, options such as a skin graft or a skin flap may be used to repair the area. If the defect is near the eyes or facial regions, an oculoplastic surgeon may be involved in the reconstruction to restore both function and appearance. Some extensive reconstructive procedures may be performed in an operating room under sedation or anesthesia to ensure optimal results.
In addition to caring for the surgical area, practicing skin cancer prevention is crucial. Protect your healthy skin by using sunscreen, wearing protective clothing, and avoiding excessive sun exposure. Regular self-examinations and routine check-ups with a dermatologist can help detect any new skin cancers early, when they are most treatable. Be sure to check all areas of your body, including the genital area, for new or unusual skin lesions. By staying vigilant and proactive, you can support your recovery and reduce the risk of future skin cancers.
The Bottom Line
For most basal cell and squamous cell carcinomas, Mohs micrographic surgery offers the highest cure rates, the greatest tissue preservation, and the best cosmetic outcomes. Its precision allows surgeons to remove every cancer cell while protecting healthy skin—an advantage especially important for facial and delicate areas.
While radiation therapy remains an important option for specific patients, it lacks the precision of Mohs surgery and carries a greater risk of long-term skin damage. Discussing your diagnosis and goals with a qualified Mohs surgeon can help determine the treatment approach that’s safest and most effective for you.
If you’ve been diagnosed with skin cancer, don’t hesitate to seek a consultation with a board-certified dermatologist or Mohs surgery specialist. Organizations such as the American Academy of Dermatology and the Dermatologic Surgery Association provide guidelines and standards for skin cancer treatment, including Mohs surgery, to ensure patients receive safe and effective care. Understanding your options is the first step toward the best possible outcome for both your health and your confidence.
For More Information…
Contact HazanyDerm. Dr. Hazany is recognized for his precision, compassion, and commitment to achieving the best aesthetic and medical outcomes for every patient. His expertise in Mohs micrographic surgery allows for complete cancer removal while preserving as much healthy tissue as possible—an approach that minimizes scarring and promotes faster, more natural healing.
At Dr. Hazany’s practice, patients receive individualized care rooted in the highest standards of dermatologic surgery. Each case is carefully evaluated to ensure that the chosen treatment plan balances optimal medical results with aesthetic considerations, particularly for sensitive areas such as the face, neck, and hands.
Whether you’re seeking a second opinion, exploring treatment options, or ready to move forward with surgery, Dr. Hazany and his team provide the clarity, reassurance, and expertise you deserve. From diagnosis to recovery, their focus remains steadfast: restoring health, confidence, and peace of mind.